Introducing our
White-Label
Online Training Platform
with Trackability
HR Proactive's White-Label Online Training Platform with trackability is a customized full-service platform to house your company's Human Resources and Health & Safety training products and documents.
Build Skills, Culture, and Compliance!

Featured Training Programs

White-Label
Learning Management System
Its ease of use is ideal for employees to access your company’s training manuals, employee handbook, health & safety manual, and other policies and procedures.
Our State-of-the-Art White-Label Online Training Platform is mobile-friendly and compatible with your smart-phone, tablet, laptop, and desktop computer.
We provide a cost-effective online solution for your training needs!
Benefits of a White-Label Training Platform
With our White-Label Online Training Platform, learners will be provided with a meaningful learning experience without knowing the training platform is from an outside source!
Customizable Features
Fully Integrated and Ready-Made Training Solution
Quick and easy to add your Brand, Logo, and Identity
Tech Supported Platform
Clear and Simple Path to Train Learners
Saves you Time and Money on Research & Development
HR Proactive Inc. has been helping organizations
build Culture and Connections with compliance training
products and services for over twenty-five years.
Quality Content
The quality breadth and timeliness of content updating is paramount to the learner process.
Learner Engagement
Motivate learners and keep them engaged in the learning experience.
User Experience
Our "People First" system helps you to assign, track, and report employee progress.
Learner Outcomes
Align compliance training with your business outcomes.
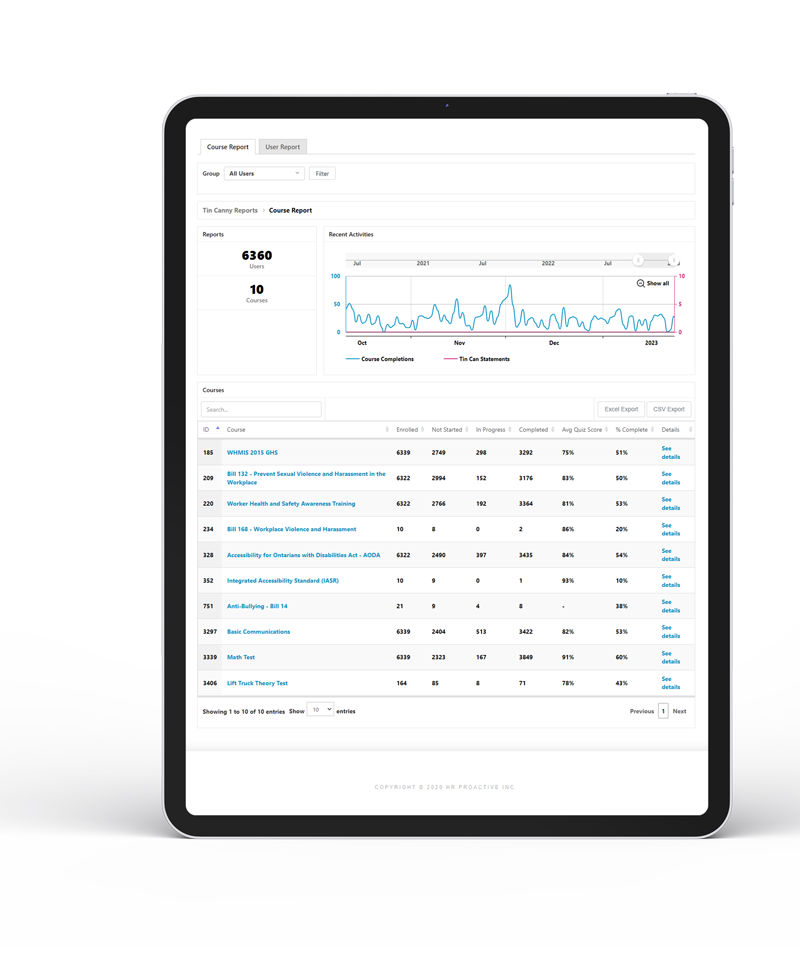
Track and report
on employee progress
We have you covered with timely reports that can be accessed real-time to ensure compliance with HR and Health & Safety legislation/training requirements.
Call us today to experience our
exceptional customer service!
- 1 (888) 552-1155
- sales@hrproactive.com
Please complete the form below and we will get back to you shortly.

